Carolinas Medical Center - Global Emergency Medicine
https://atriumhealth.org/education/graduate-medical-education/physician-fello...

We will not be accepting a new fellow in the 2021 match (to start in 2022), as all fellowship spots for the 2022 - 2023 academic year are full. We will once again be recruiting a fellow for the 2022 match to start in the summer of 2023.
The Department of Emergency Medicine at Carolinas Medical Center has a strong commitment to expanding emergency care for the sick and wounded globally. Our global emergency medicine (GEM) program operates under the mission of capacity and resilience building and international crisis response. As part of these efforts, we launched a Global EM fellowship in July 2018, and graduated our first fellow in June 2019.
Since 2009, our department has enjoyed a productive clinical and research capacity-building relationship with a major teaching hospital and affiliated university in Dar es Salaam, Tanzania: Muhimbili National Hospital (MNH) and the Muhimbili University of Health and Allied Sciences (MUHAS). The tangible products of this collaboration include the development of the MNH ED and the emergency medicine residency program at MUHAS. Both the ED and the residency program are the first of their kind in Tanzania and both are now staffed and run by locally-trained emergency physicians and nurses. To date, the research products of our inter-institutional collaboration have included 16 scientific abstract presentations (14 by a Tanzanian investigator) and nine full-length peer-reviewed publications (5 with a Tanzanian first author and all with a Tanzanian second author). Our approach to this partnership has focused on sustainability and so all our research and educational activities are aimed at building local capacity. The emergency care in Tanzania is led by the Emergency Medical Association of Tanzania (EMAT).
The Department of Emergency Medicine also has a partnership with the disaster response, non-profit organization, Team Rubicon, with medical direction being provided by the Department of Emergency Medicine at CMC. 70% of Team Rubicon’s 75,000 volunteers are military veterans, allowing the organization to respond quickly and efficiently to disaster areas in the United States and internationally. Pairing the skills of military veterans with first responders and emergency medical personnel Team Rubicon can respond to international disaster responses.
The GEM fellowship is a 12 – 24-month fellowship. Fellows in the 24-month track have the option to pursue either a Master's of Science in Public Health Degree or a Diploma in Tropical Medicine and Hygiene (DTMH).
The Department of Emergency Medicine at Carolinas Medical Center has a strong commitment to expanding emergency care for the sick and wounded globally. Our global emergency medicine (GEM) program operates under the mission of capacity and resilience building and international crisis response. As part of these efforts, we launched a Global EM fellowship in July 2018, and graduated our first fellow in June 2019.
Since 2009, our department has enjoyed a productive clinical and research capacity-building relationship with a major teaching hospital and affiliated university in Dar es Salaam, Tanzania: Muhimbili National Hospital (MNH) and the Muhimbili University of Health and Allied Sciences (MUHAS). The tangible products of this collaboration include the development of the MNH ED and the emergency medicine residency program at MUHAS. Both the ED and the residency program are the first of their kind in Tanzania and both are now staffed and run by locally-trained emergency physicians and nurses. To date, the research products of our inter-institutional collaboration have included 16 scientific abstract presentations (14 by a Tanzanian investigator) and nine full-length peer-reviewed publications (5 with a Tanzanian first author and all with a Tanzanian second author). Our approach to this partnership has focused on sustainability and so all our research and educational activities are aimed at building local capacity. The emergency care in Tanzania is led by the Emergency Medical Association of Tanzania (EMAT).
The Department of Emergency Medicine also has a partnership with the disaster response, non-profit organization, Team Rubicon, with medical direction being provided by the Department of Emergency Medicine at CMC. 70% of Team Rubicon’s 75,000 volunteers are military veterans, allowing the organization to respond quickly and efficiently to disaster areas in the United States and internationally. Pairing the skills of military veterans with first responders and emergency medical personnel Team Rubicon can respond to international disaster responses.
The GEM fellowship is a 12 – 24-month fellowship. Fellows in the 24-month track have the option to pursue either a Master's of Science in Public Health Degree or a Diploma in Tropical Medicine and Hygiene (DTMH).
Clinical Sites
Home Institution: Carolinas Medical Center Main (CMC) in Charlotte, North Carolina. CMC is an 874-bed, community-based, tertiary care teaching hospital that serves as the only regional level-I trauma center, the State Poison Control Center, and is a tertiary referral center for Mecklenburg County and 16 surrounding counties in North and South Carolina. It is the flagship facility for the network that includes acute care facilities, subacute facilities, and clinics in North and South Carolina. The campus includes an adjacent 234-bed children's hospital, Levine Children's hospital, which is a Pediatric Level 1 trauma center. Residency programs exist in all specialties including Emergency Medicine, which is a PGY 1-3 program that includes 42 residents. Fellowship positions are offered in EMS, Toxicology, Ultrasound, Pediatric Emergency Medicine, and Disaster and Operational medicine. There are 41 academic faculty members in the Department of Emergency Medicine as well as 2 adjunct assistant professors in the Department of Emergency Medicine from Muhimbili National Hospital in Dar es Salaam, Tanzania. The Emergency Department at Carolinas Medical Center manages over 115,000 patients each year, or about 300 to 320 patients per day. The department features an unusually diverse mix of patient care opportunities, and the socioeconomic diversity of our patient population sets us apart from other institutions. CMC ED physicians work in one of three adult treatment areas to which patients are triaged by acuity of illness, as well as a 21-bed Children's ED. The Children's ED is first in the region that offers 24-hour emergency care for children in a family-centered environment. Three to six board-certified emergency medicine faculty members are present in the open areas 24-hours a day.
CMC Global EM fellows will be classified as junior EM faculty and will work clinical shifts in the CMC ED as the attending physician. In this capacity, their responsibilities will include delivery of clinical patient care as well as the supervision and education of CMC residents and advanced care providers.
International Partner Sites:
Emergency Medicine Department, Muhimbili National Hospital (MNH), Dar es Salaam, Tanzania. MNH opened the first public, full service ED in Tanzania in 2009, and now sees a daily volume of 150-200 patients (20% pediatrics). In 2021, a new dedicated pediatric emergency department opened on the same campus. Specialty clinics attend 1000 patients a day, and the hospital has a bed capacity of 1500 patients. All specialties are available at the MNH Campus including medical, surgical, cardiovascular, trauma, pediatrics, and psychiatry. Fellows wishing to treat patients will become licensed physicians in Tanzania. Medical licensure will be provided by the Medical Council of Tanzania for fellows wishing to treat patients. The Emergency Medicine Department at MNH is led by locally-trained specialists in Emergency Medicine who are available to provide mentorship.
Hospital Regional de Escuintla, Escuintla, Guatemala. In a unique collaboration between the Pediatrics department of the Hospital Regional de Escuintla, the Pediatrics and Emergency Medicine departments at CMC, we have developed an ultrasound training program for Escuintla's Pediatrics residents. In addition to ongoing ultrasound educational projects including "Train the trainer" courses for local pediatric attending physicians, CMC EM faculty are researching novel uses of ultrasound in low resource settings. We have also expanded ultrasound training to general surgery residents in Escuintla.
San Juan de Dios Hospital, Guatemala City, Guatamala. CMC EM Faculty in the ultrasound division successfully secured grant funding for an ultrasound machine that was donated to the recently established EM Residency Program at IGSS in Guatemala City. The first in-depth critical care ultrasound course for these residents took place in November 2021.
Team Rubicon, USA
CMC Global EM fellows will be classified as junior EM faculty and will work clinical shifts in the CMC ED as the attending physician. In this capacity, their responsibilities will include delivery of clinical patient care as well as the supervision and education of CMC residents and advanced care providers.
International Partner Sites:
Emergency Medicine Department, Muhimbili National Hospital (MNH), Dar es Salaam, Tanzania. MNH opened the first public, full service ED in Tanzania in 2009, and now sees a daily volume of 150-200 patients (20% pediatrics). In 2021, a new dedicated pediatric emergency department opened on the same campus. Specialty clinics attend 1000 patients a day, and the hospital has a bed capacity of 1500 patients. All specialties are available at the MNH Campus including medical, surgical, cardiovascular, trauma, pediatrics, and psychiatry. Fellows wishing to treat patients will become licensed physicians in Tanzania. Medical licensure will be provided by the Medical Council of Tanzania for fellows wishing to treat patients. The Emergency Medicine Department at MNH is led by locally-trained specialists in Emergency Medicine who are available to provide mentorship.
Hospital Regional de Escuintla, Escuintla, Guatemala. In a unique collaboration between the Pediatrics department of the Hospital Regional de Escuintla, the Pediatrics and Emergency Medicine departments at CMC, we have developed an ultrasound training program for Escuintla's Pediatrics residents. In addition to ongoing ultrasound educational projects including "Train the trainer" courses for local pediatric attending physicians, CMC EM faculty are researching novel uses of ultrasound in low resource settings. We have also expanded ultrasound training to general surgery residents in Escuintla.
San Juan de Dios Hospital, Guatemala City, Guatamala. CMC EM Faculty in the ultrasound division successfully secured grant funding for an ultrasound machine that was donated to the recently established EM Residency Program at IGSS in Guatemala City. The first in-depth critical care ultrasound course for these residents took place in November 2021.
Team Rubicon, USA
David Callaway, MD, serves as the Chief Medical Officer and Medical Director for Team Rubicon (TR). In June 2018, Team Rubicon became the first US-based NGO to become certified as an Emergency Medical Team, Type I Mobile by the World Health Organization (WHO). Previous CMC fellows have been deployed internationally for capacity-building work and sudden-onset and complex humanitarian emergencies in the following countries: Uganda, Papau New Guinea, The Bahamas, Mozambique, Mariana Islands, Greece.
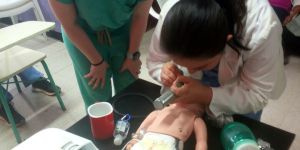

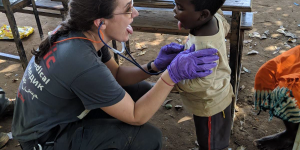
Fellowship Curriculum Outline
Clinical Care Average 12 hours/week clinical responsibility over the academic year for 49 weeks with 2 weeks of vacation and 1 week of CME. Clinical responsibilities will be blocked to allow for longer international experiences.
One-Year Track: Educational Blocks:
1. Travel and Field Medicine – Two months
a. Course - CMC Global Heath Intensive Course, Charlotte NC (2 weeks) (Participant role)
2. Disaster Management - Two Months
a. Recommended Course - FEMA Barrier Precautions and Controls for Highly Infectious Disease, Anniston, Alabama (4 days)
3. EM Systems and Development – Two Months
4. Public Health – Two Months
5. Humanitarian Relief – Two months
a. Course – Harvard Humanitarian Initiative (2 weeks)
6. Program Administration – Two months
a. Optional Course - SAEM grant-writing workshop
7. Academic Skills – Longitudinal
8. Global Health Ethics – Longitudinal
Two-Year Track (example, with Master’s in Science in Public Health Degree): Educational Blocks
1. Travel and Field Medicine I – Two months
a. Course - CMC Global Heath Intensive Course, Charlotte NC (2 weeks) (Participant role)
2. Disaster Management - 4 months
a. Recommended Course - FEMA Barrier Precautions and Controls for Highly Infectious Disease, Anniston, Alabama (4 days)
3. Humanitarian Relief – 4 months
a. Course – Harvard Humanitarian Initiative (2 weeks)
4. Program Administration & Research I – 3 months
a. Optional Course - SAEM grant-writing workshop
5. Academic Skills/Becoming a Master Educator – 3 months
a. Course – CMC Global Health Intensive Course, Charlotte NC (Instructor role)
6. Travel and Field Medicine Block II – 2 months
7. EM Systems and Development – 2 months
8. Program Administration & Research Block II – 4 months
9. Public Health - Longitudinal (per Master’s degree curriculum))
10. Ethics in Global Health - Longitudinal
Fellow Didactics - will be on Tuesdays when the fellow is in Charlotte.
Journal Clubs - will be every 3 months and organized by the fellow.
Courses
1. Choice of:
a. Humanitarian Emergencies in Large Populations (HELP), Honolulu Hawaii, Summer 2023 or 2024 - OR -
b. Humanitarian Response Intensive Course, Boston Massachusetts, Spring 2024
2. Global Health Intensive Course at CMC (Summer 2023)
3. Additional CME funding available for additional conference activities of the fellow's choosing, including SAEM, SAEM's grant writing workshop, ACEP, Consortium of Universities for Global Health, and Basic Emergency Care training courses.
Electives/International Experience
1. Muhimbili National Hospital Emergency Department, Dar es Salaam, Tanzania - up to 3 months/year
2. Escuintla Hospital, Escuintla, Guatemala, 2 weeks/year of optional projects in ultrasound education
3. Team Rubicon USA, International medical disaster response, approximately - multiple weeks per year based on disaster response needs when organization is responding to international disaster
Projects
| Project Name & Description | Details |
|---|
Alumni
Contacts
Program Director

Adeline Dozois
Director of Global Emergency Medicine at Carolinas Medical Center. Dr. Dozois has experience working in diverse settings across Africa, South Ameri...
Application
Beginning in the fall 2022, we will once again be recruiting a fellow for the 2022 match to start in the summer of 2023.
Application Process
To apply, upload the following documents to the GEMF Website 1. CV 2. Personal statement: including interest in our program, experience, and goals 3. 2 letters of reference
In your application email, please indicate whether you would like to be considered for the 12-month track, the 24-month track, or both. If both, please indicate which track is preferred.
Important Dates
Application Deadline : Oct 01, 2022
This application deadline refers to the 2022 Match